🇫🇷 Lire en Français | 🇪🇸Leer en Español | 🇧🇷Leia em português
Imagine purchasing a beautiful, healthy-looking dog to strengthen your breeding program. She passes every visual health check, cycles normally, and breeds without difficulty. Then, at 50 days of gestation, she aborts an entire litter. A dark, foul-smelling vaginal discharge persists for weeks. Before you understand what happened, two more females in your facility lose their litters. Your stud dog develops swollen testicles and his semen quality plummets.
When your veterinarian finally runs the right test, the diagnosis is devastating: canine brucellosis. The bacteria that caused this — Brucella canis — hides inside your dog’s own cells, making it virtually impossible to cure with antibiotics. As a veterinarian, I have seen the heartbreak this disease causes. But I have also seen breeders who prevent it through proactive testing and biosecurity. This article gives you the complete playbook.
- TL;DR: Key Takeaways
- What Should You Know About Canine Brucellosis?
- What Should You Do If Brucellosis Is Suspected?
- What Should You Have Ready for Prevention?
- What Warning Signs Should You Watch For?
- Your Best Defense Is the One You Build Before You Need It
TL;DR: Key Takeaways
- Test all active breeding stock every 3 to 6 months and before every mating — routine screening is your first line of defense.
- A healthy-looking dog can silently spread Brucella canis through mating, aborted materials, urine, and even artificial insemination with fresh or frozen semen.
- The hallmark sign is late-term abortion between days 45 and 59, but many infected dogs show no symptoms while spreading bacteria to your entire kennel.
- The bacteria hides inside immune cells, making antibiotic treatment rarely curative — relapses occur within 3 to 6 months in most treated dogs.
- New dogs must complete strict quarantine with two negative tests spaced 4 to 6 weeks apart before joining your breeding population.
- This is zoonotic — breeders and kennel staff can catch it through contact with birthing fluids, aborted material, or urine. Wear PPE.
What Should You Know About Canine Brucellosis?
The Bacteria That Hides Inside Your Dog’s Cells
Brucella canis is a stealthy bacterium classified as a “rough” strain of Brucella. Think of it as a microscopic burglar that breaks into your dog’s immune cells — the very cells designed to destroy invaders — and sets up permanent residence. Once inside the macrophages, it replicates in a low-pH environment that shields it from the immune system and from most antibiotics. This intracellular hiding strategy explains everything: why treatment rarely works, why relapses are common, and why there is currently no cure.
After initial infection, the bacteria spread through the blood and lymphatic system, showing a powerful preference for reproductive organs — the uterus, placenta, testes, and prostate. They can survive up to 2 months in organic debris, making contaminated whelping areas a persistent hazard until properly disinfected.
| Characteristic | Detail | Why It Matters for Breeders |
|---|---|---|
| Classification | Gram-negative, rough-strain Brucella | Standard livestock brucellosis tests will NOT detect it |
| Survival strategy | Hides inside host macrophages (immune cells) | Antibiotics cannot reliably reach and kill it |
| Organ preference | Uterus, placenta, testes, prostate, lymph nodes | Causes reproductive failure in both sexes |
| Environmental survival | Up to 2 months in organic debris | Whelping areas remain infectious without proper disinfection |
| Infectious dose | As low as 10,000 organisms via eye contact | Extremely easy to transmit in a kennel environment |
How It Spreads Through Your Facility
Brucella canis spreads through every route a breeder fears most. Venereal transmission during natural mating is a primary pathway, but here is the detail that shatters a common misconception: artificial insemination does not protect you. The bacteria survives in fresh, chilled, and frozen semen. A stud dog can look perfectly healthy and silently transmit it to every female inseminated with his semen.
The oronasal route is equally dangerous. Post-abortion vaginal discharge contains up to 10 billion bacteria per milliliter (mL) — the single most concentrated source of infection. The bacteria also shed in urine (especially from males), milk, and saliva. Many infected dogs remain completely asymptomatic while silently contaminating your entire facility.
| Transmission Route | Source Material | Risk Level | Prevention Strategy |
|---|---|---|---|
| Venereal (natural mating) | Semen, vaginal secretions | Very high | Test both dogs before every mating |
| Artificial insemination | Fresh, chilled, or frozen semen | High | Require negative test from semen donor |
| Oronasal contact | Vaginal discharge, urine, saliva | High | Isolate new dogs; clean shared surfaces |
| Aborted material | Fetal tissue, placenta, fluids | Extremely high | Wear PPE; dispose of material safely |
| Transplacental | Mother to puppies in utero | High | Test all breeding females before mating |
| Fomites (contaminated objects) | Bedding, equipment, kennel surfaces | Moderate | Disinfect with 2.5% bleach; 10-minute contact time |
Why Standard Tests Can Mislead You
The most common screening test — the Rapid Slide Agglutination Test (RSAT) — is highly sensitive but has a specificity of only about 83%. It catches most infections early (within 2 to 4 weeks) but produces false-positive results in up to 60% of positive screens. Cross-reactions with Bordetella bronchiseptica (kennel cough), Pseudomonas, and Staphylococcus are the primary culprits.
This is why canine brucellosis diagnosis requires a serial testing approach. A positive screen must always be confirmed with a more specific test: the 2ME-RSAT, AGID, Cornell’s Canine Brucella Multiplex (CBM), or bacterial culture with PCR. One reassurance: your dog’s leptospirosis vaccination will not cause a false positive. Never make breeding or euthanasia decisions based on a single screening test alone.
| Test | What It Detects | Timing | Limitation |
|---|---|---|---|
| RSAT (screening) | Antibodies against B. canis surface antigens | Positive 2–4 weeks post-infection; results in 2 minutes | Low specificity (~83%); up to 60% false-positive rate |
| 2ME-RSAT (confirmatory) | IgG antibodies only (destroys cross-reacting IgM) | Best after 8–12 weeks post-infection | May miss early infections when only IgM is present |
| AGID (confirmatory) | Antibodies to internal cytoplasmic proteins | Positive 8–12 weeks post-infection | High specificity but slower to become positive |
| Cornell CBM (multiplex) | Multiple antibody targets simultaneously | Can detect early and established infections | Requires submission to specialized laboratory |
| Blood culture (gold standard) | Live Brucella organisms from blood | Best 2–4 weeks post-infection (peak bacteremia) | Bacteremia is intermittent; requires 3 consecutive cultures 24 hours apart |
| PCR | Brucella DNA in blood, semen, urine, or vaginal swabs | Any stage of infection | A negative PCR does not rule out infection (intermittent shedding) |
What Should You Do If Brucellosis Is Suspected?
Implement a Routine Screening Protocol
Prevention is your strongest weapon because canine brucellosis has no reliable cure. Work with your veterinarian to establish a screening schedule: test all active breeding stock every 3 to 6 months using the RSAT. Test every dog before every breeding event — natural mating or AI. For shipped semen from an outside stud, require documentation of a negative test taken within 30 days of collection.
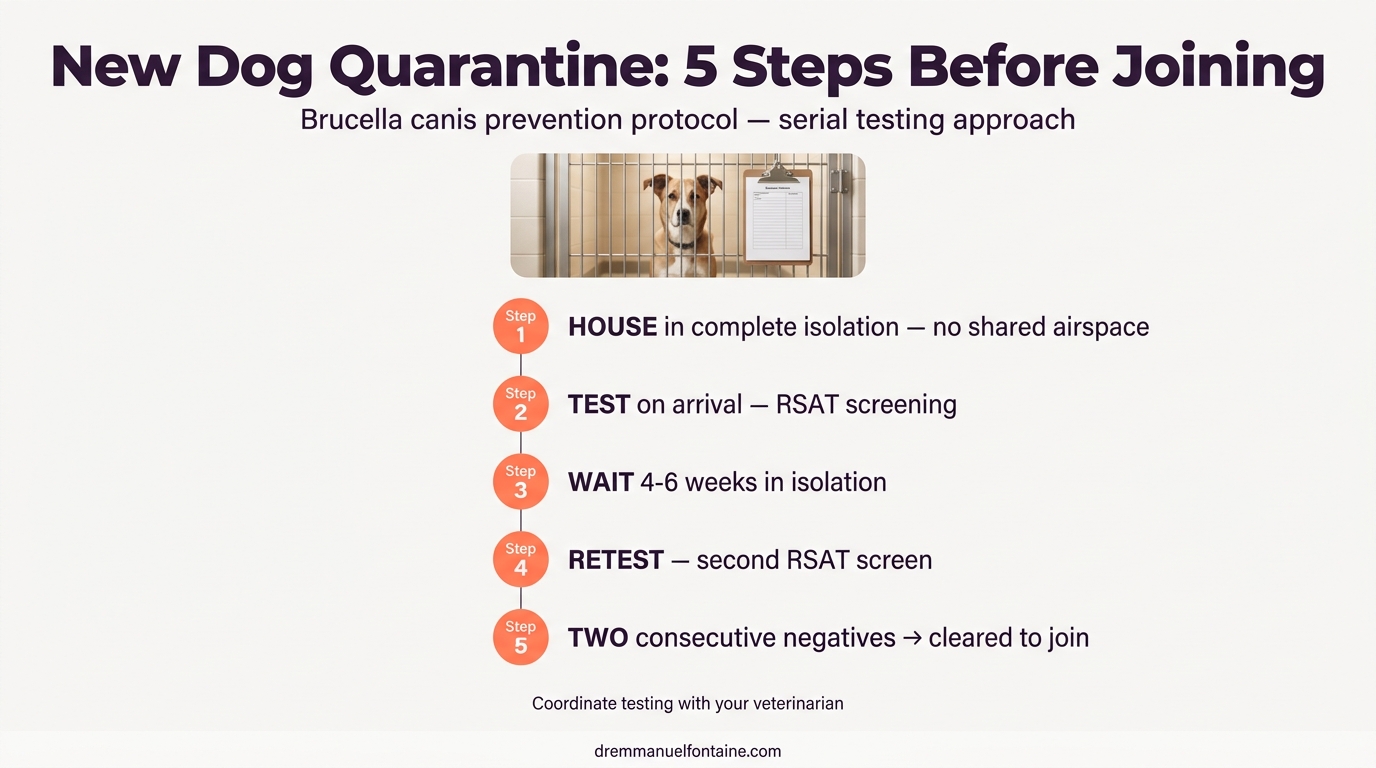
For any new dog entering your facility, enforce an absolute quarantine protocol. House the newcomer in complete isolation and run an initial RSAT on arrival, then retest 4 to 6 weeks later. Only after two consecutive negative results should that dog join your breeding population. This two-test protocol accounts for the incubation period: a dog tested too early after exposure may have a falsely negative result.
| Scenario | Test Required | Frequency | Action if Positive |
|---|---|---|---|
| Active breeding stock | RSAT or equivalent screen | Every 3–6 months | Isolate immediately; run confirmatory test |
| Before every mating | RSAT on both dogs | Each breeding event | Cancel breeding; retest in 4–6 weeks |
| New dog entering facility | RSAT on arrival + retest at 4–6 weeks | Two tests before joining population | Keep in quarantine; run confirmatory test if positive |
| Outside stud (shipped semen) | Negative test within 30 days of collection | Per semen shipment | Reject shipment; request new test documentation |
| Post-abortion investigation | RSAT + confirmatory test (2ME-RSAT, AGID, or PCR) | Immediately after event | Quarantine entire facility; test all dogs |
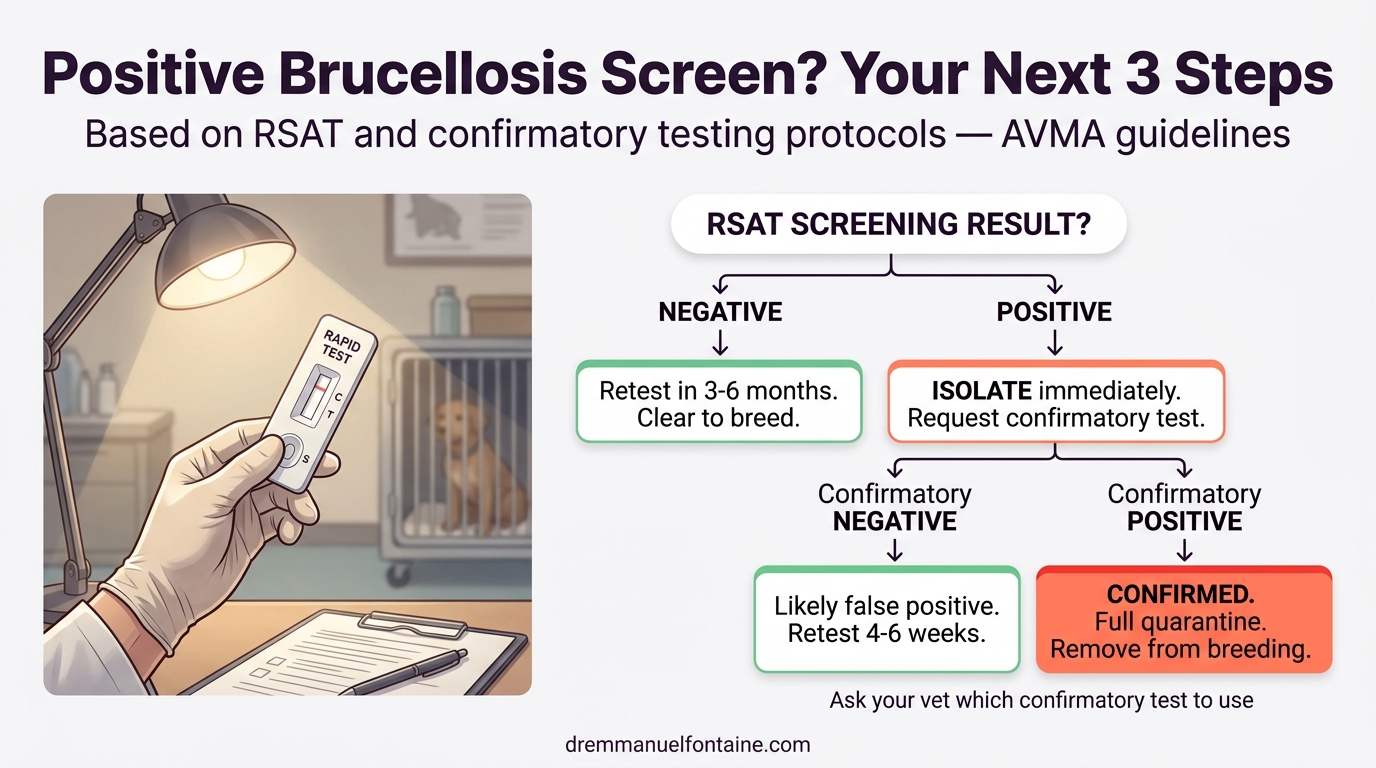
Respond Immediately to a Positive Result
If a screening test returns positive, do not panic — but act immediately. As discussed in WHAT TO KNOW, the RSAT has a high false-positive rate, so a single positive screen does not confirm infection. However, isolate the suspect dog right away and request confirmatory testing: 2ME-RSAT, AGID, Cornell CBM, or blood culture with PCR.
If confirmed positive, the situation becomes critical. Work with your vet and state animal health authorities — this is a reportable disease in many states. Place the entire facility under quarantine. The confirmed-positive dog must be permanently removed from the breeding program through surgical sterilization with lifelong isolation. All remaining dogs must test negative every 30 days for 3 consecutive rounds before quarantine can be lifted.
| Test Result | Status | Immediate Action | Next Step |
|---|---|---|---|
| RSAT positive, 2ME-RSAT negative | Possible early infection or false positive | Maintain isolation of suspect dog | Retest in 4–6 weeks; do not breed |
| RSAT positive, confirmatory positive | Confirmed infection | Full facility quarantine; remove dog from breeding | Report to state authorities; test all kennel dogs monthly |
| All kennel dogs test negative (3 rounds) | Quarantine eligible for release | Continue monitoring every 3–6 months | Maintain strict intake quarantine for new dogs |
| Treated dog (pet, not breeding) | Lifelong carrier risk | Spay/neuter; isolate from breeding dogs | Monitor with AGID every 2–6 months indefinitely |
Protect Yourself — This Disease Affects Humans Too
Brucella canis is zoonotic — it spreads from dogs to humans. Breeders, kennel staff, and veterinary personnel are at the highest occupational risk through direct contact with aborted materials, birthing fluids, or urine. Pregnant women, children, and immunocompromised individuals are especially vulnerable.
When handling whelping materials or cleaning areas used by suspect dogs, wear full personal protective equipment: disposable gloves, eye protection, waterproof gown, and shoe covers. Anyone exposed to a confirmed-positive dog should consult their healthcare provider and should not donate blood for 6 months.
| Protection Measure | When to Use | Why It Matters |
|---|---|---|
| Disposable gloves | Handling any dog during whelping; cleaning kennel areas | Prevents skin contact with contaminated fluids |
| N95 respirator | Handling aborted material; cleaning contaminated areas | Blocks inhalation of aerosolized bacteria |
| Eye protection / face shield | Assisting births; handling urine or vaginal discharge | Prevents conjunctival infection (very low infectious dose via eyes) |
| Waterproof gown / coveralls | Any direct contact with suspect or positive dogs | Prevents clothing contamination; limits spread between areas |
| Shoe covers | Entering isolation or whelping areas | Prevents carrying bacteria on footwear to clean areas |
| Healthcare consultation | After any exposure to confirmed-positive dog or fluids | Early detection of human brucellosis enables effective treatment |
What Should You Have Ready for Prevention?
Diagnostic Access and Laboratory Relationships
Your most important preparation is a relationship with a diagnostic laboratory offering the full range of B. canis testing. Cornell’s Animal Health Diagnostic Center, for example, offers the Canine Brucella Multiplex (CBM), 2ME-RSAT, and AGID II. Your vet should know which lab to use and which tests to request at each stage of the diagnostic process.
For point-of-care screening, the Zoetis D-Tec CB RSAT was the historical standard but was discontinued in 2022. Current options include the Bionote Anigen Rapid C.Brucella Ab lateral flow assay and the VMRD IFA test. Ask your vet which screening platform they use — speed matters when you need to isolate a suspect dog.
| Resource | What It Provides | When You Need It |
|---|---|---|
| In-house RSAT or lateral flow kit | Rapid screening (results in 2 minutes to same day) | Routine screening; pre-breeding checks; new dog arrivals |
| Diagnostic laboratory (Cornell, state lab) | Confirmatory tests: 2ME-RSAT, AGID, CBM, culture, PCR | After any positive screening result |
| Veterinary ultrasound | Detection of prostatic enlargement or testicular abscesses | When stud dogs show scrotal swelling or pain |
| Radiography / MRI | Diagnosis of diskospondylitis (spinal infection) | When dogs show back pain, lameness, or neurological signs |
| Semen analysis | Detection of head-to-head agglutination, abnormal morphology | Routine stud dog evaluation; declining fertility investigation |

Quarantine Infrastructure and Biosecurity Supplies
Every facility needs a dedicated isolation area physically separated from the main kennel — no shared airspace, drainage, or equipment. New arrivals, dogs returning from outside matings, and any suspect dog must be housed here.
Stock disinfection supplies to neutralize the bacteria. It is easily killed by common disinfectants, but only after removing organic material first. Use 2.5% sodium hypochlorite (bleach), 70% ethanol, or quaternary ammonium compounds with a minimum 10-minute wet contact time. For equipment sterilization, use autoclaving at 121 °C (250 °F) for 15 minutes, or dry heat at 160–170 °C (320–338 °F) for 1 hour.
| Category | Items | Specification |
|---|---|---|
| Disinfectants | Sodium hypochlorite (bleach) | 2.5% concentration; 10-minute wet contact time |
| Disinfectants | 70% ethanol or quaternary ammonium compounds | Alternative disinfectants; same 10-minute contact time |
| PPE | Gloves, N95 masks, eye protection, gowns, shoe covers | Disposable; dedicated to isolation area |
| Isolation housing | Separate kennel runs or cages | No shared drainage, airspace, or equipment with main kennel |
| Heat sterilization | Autoclave or oven access | 121 °C (250 °F) for 15 min (moist) or 160–170 °C (320–338 °F) for 1 hour (dry) |
| Waste disposal | Double-bagged biohazard waste bags | For aborted material, contaminated bedding, used PPE |
Regulatory Contacts and Emergency Protocols
Know your regulatory landscape before a crisis strikes. As noted iearlier, this is a reportable disease in many states, meaning your vet must notify authorities if a case is confirmed. Identify your state veterinarian’s office and understand quarantine requirements — some states mandate monthly testing until 3 consecutive negative rounds; others require testing every 90 days.
Have a written emergency response plan that includes: your vet’s emergency contact, the nearest diagnostic lab, your state reporting hotline, a pre-positioned isolation area with PPE, and a communication plan for puppy buyers and co-breeders who may have received dogs or semen from your facility.
| Contact / Protocol | Purpose | When to Activate |
|---|---|---|
| Primary veterinarian (direct line) | Clinical assessment, testing, treatment decisions | Any reproductive failure or positive screening test |
| Diagnostic laboratory | Confirmatory testing (2ME-RSAT, AGID, CBM, PCR) | Immediately after any positive RSAT screen |
| State veterinarian / animal health authority | Regulatory reporting and quarantine mandates | Upon confirmed positive diagnosis |
| Facility quarantine protocol | No dogs enter or leave; monthly testing begins | Confirmed positive in any dog on premises |
| Communication plan for co-breeders/buyers | Notify anyone who received dogs or semen from your facility | Upon confirmed positive; legal and ethical obligation |
What Warning Signs Should You Watch For?
Subtle Early Signs You Must Not Ignore
Many infected dogs show no obvious signs. In females, the earliest indicator is often unexplained conception failure — early embryonic death around 10 to 35 days post-conception mimics a “missed breeding.” If a proven female repeatedly fails to conceive despite normal cycles, B. canis testing should be on your differential list.
In males, watch for moist scrotal dermatitis, mild epididymal swelling, or scrotal edema. Semen analysis is the earliest diagnostic window — abnormal sperm appear as early as 2 weeks post-infection, and by 20 weeks, up to 90% may show head-to-head agglutination. Non-specific signs like lethargy, poor coat, and enlarged lymph nodes can also appear but are easily attributed to other causes.
| Sign | Sex Affected | What It May Indicate | Your Action |
|---|---|---|---|
| Repeated conception failure | Females | Early embryonic death from B. canis infection | Request B. canis screening (RSAT) |
| Moist scrotal dermatitis | Males | Epididymitis or orchitis from early infection | Veterinary examination; semen analysis; RSAT |
| Abnormal semen (head-to-head agglutination) | Males | Active B. canis infection of reproductive tract | Immediate isolation; full diagnostic workup |
| Enlarged lymph nodes | Both | Systemic immune response to Brucella infection | RSAT screening; physical examination by vet |
| Lethargy, weight loss, poor coat | Both | Non-specific but consistent with chronic brucellosis | RSAT if other causes are ruled out |
Emergency Red Flags Demanding Immediate Vet Contact
The hallmark emergency sign of canine brucellosis is late-term abortion between days 45 and 59 of gestation. Any abortion in this window should immediately trigger testing. The aborted material and vaginal discharge — dark, fetid, and gray-green — persist for 1 to 6 weeks and contain up to 10 billion organisms per mL. Handle all aborted material with the full PPE described in the WHAT TO DO section.
Beyond reproductive signs, watch for systemic indicators. Diskospondylitis (spinal disk infection) causes severe back pain, lameness, or neurological deficits — a veterinary emergency. Recurrent uveitis (eye inflammation) with squinting or constricted pupils is another red flag. Stillborn puppies or weak neonates dying shortly after birth should also prompt immediate testing.
| Red Flag | Timing / Context | Immediate Action |
|---|---|---|
| Late-term abortion (days 45–59) | During pregnancy | Full PPE; collect samples; contact vet for B. canis testing |
| Dark, persistent vaginal discharge (1–6 weeks) | Post-abortion or post-whelping | Isolate female; test for brucellosis; handle discharge with PPE |
| Stillborn or rapidly fading neonates | At or shortly after birth | Test dam for B. canis; handle neonates with gloves |
| Severe back pain, lameness, neurological signs | Any time | Veterinary emergency; imaging for diskospondylitis |
| Recurrent eye inflammation (uveitis) | Any time | Veterinary ophthalmologic exam; test for brucellosis |
| Sudden testicular swelling then atrophy | Progressive over weeks to months | Isolate male; semen analysis; RSAT and confirmatory testing |

Signs That Treatment Is Working — or Failing
If treatment is attempted for a pet dog (confirmed-positive dogs must be permanently removed from breeding), monitoring is a long-term commitment. Signs of treatment success include resolving clinical signs and consecutive negative bacterial cultures. Serological clearance requires two consecutive negative AGID tests spaced 2 to 6 months apart — in successful cases, dogs reached seronegative status after a median of 96 weeks of continuous combination antibiotic therapy.
Relapses typically occur within 3 to 6 months after stopping antibiotics. Indicators of failure include returning clinical signs, persistent bacteremia, or titers remaining at or above 1:200 despite months of medication. A critical warning: a bitch who aborts, then delivers a healthy litter, then fails again is a persistent reservoir and must never be bred again.
| Indicator | Treatment Working | Treatment Failing |
|---|---|---|
| Clinical signs | Back pain, uveitis, or swelling resolving | Signs persist or return after stopping medication |
| Bacterial culture | Consecutive negative blood cultures | Positive cultures persist or recur |
| AGID serology | Two consecutive negatives, 2–6 months apart | Titers remain ≥1:200 or increase over time |
| Timeline to clearance | Median 96 weeks of continuous therapy | Relapse within 3–6 months of stopping antibiotics |
| Reproductive history | N/A (breeding permanently discontinued) | Intermittent litter success then failure = persistent carrier |
| Urine shedding | Decreasing or undetectable on PCR | Continued bacterial shedding in urine despite treatment |

Want to put all of this into action in your kennel? Inside the Breeder Vault, you’ll find the Canine Brucellosis Field Protocol — a printable screening schedule, quarantine checklist, decision tree for interpreting test results, and veterinary request scripts designed to be used the moment a suspect case appears. It’s the operational companion to everything you just learned.
Your Best Defense Is the One You Build Before You Need It
Canine brucellosis is silent, incurable, and zoonotic — but it is also entirely preventable. Every breeder who implements routine testing, enforces strict quarantine, and works closely with their veterinarian is building a firewall around their program.
You now understand how this pathogen operates, how it spreads, and why screening tests can mislead without proper follow-up. Partner with your vet, test consistently, quarantine rigorously, and protect your kennel with the same dedication you pour into every litter you raise.

One thought on “How to Protect Your Kennel From Brucellosis”